Did you know that the female reproductive glands play a crucial role in the intricate tapestry of reproductive health? Understanding the anatomy of these glands-such as the ovaries, fallopian tubes, and uterus-can empower you on your personal fertility journey. Whether you’re seeking to conceive, navigating challenges, or exploring options like IVF or adoption, knowing how these structures function is essential. This exploration not only enhances reproductive well-being but also addresses the emotional landscape of family building, allowing for informed decisions and realistic expectations. Join us as we dive into the fascinating world of the female reproductive glands and uncover their significance in our lives, with compassion and clarity guiding our discussion.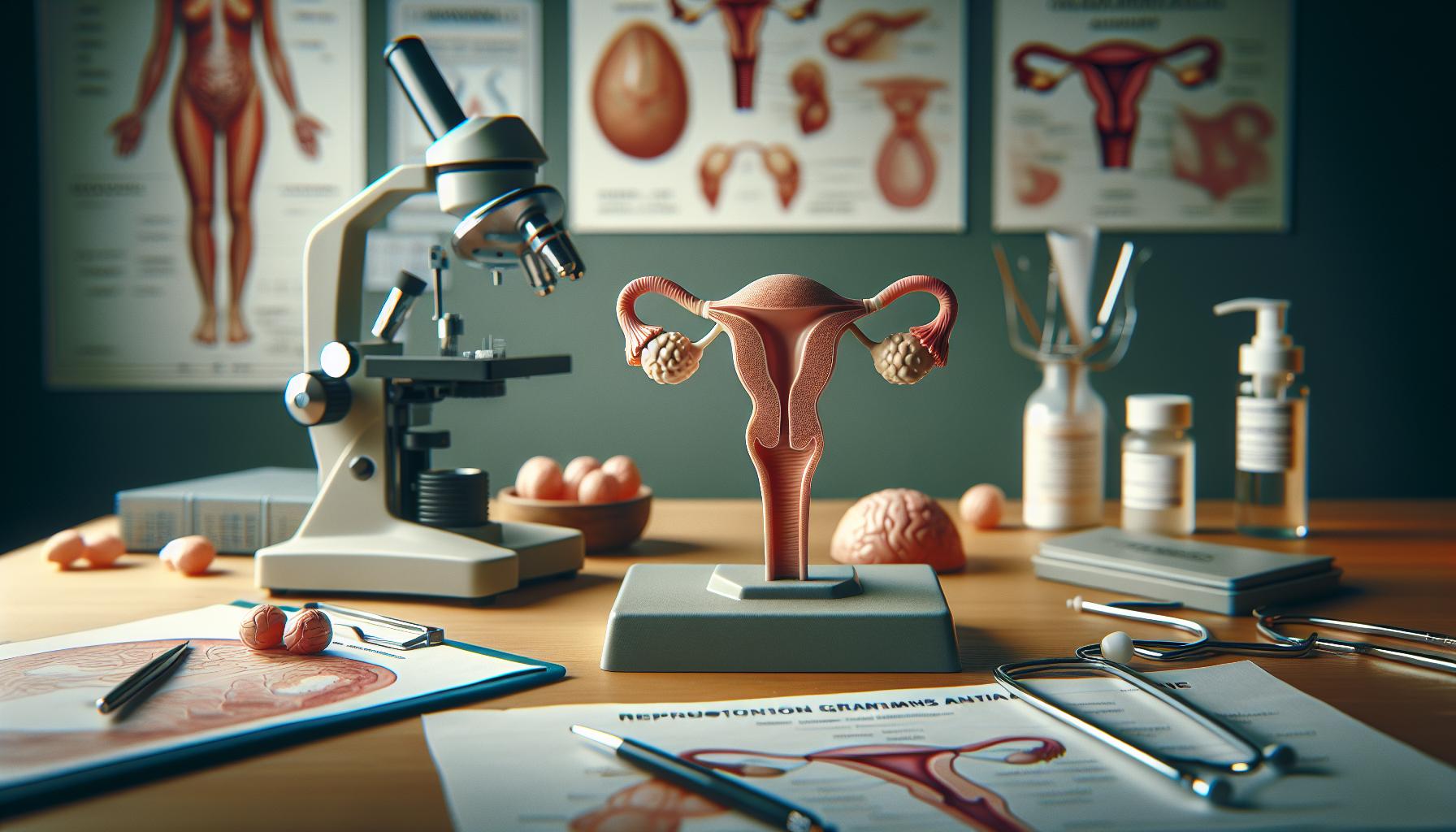
Understanding the Female Reproductive Glands
The female reproductive system is a remarkable network of glands and organs, intricately designed to facilitate reproduction and hormonal regulation. Understanding these components is crucial for appreciating their roles in fertility, menstruation, and overall health. The primary glands involved are the ovaries, which produce eggs and hormones; the pituitary gland, which regulates hormone levels; and the adrenal glands, which contribute to the hormonal balance necessary for reproductive functions.
In the ovaries, eggs are stored in structures called follicles, which also release hormones like estrogen and progesterone, critical for regulating the menstrual cycle and preparing the uterus for potential pregnancy. The pituitary gland, located at the base of the brain, releases hormones such as FSH (follicle-stimulating hormone) and LH (luteinizing hormone) that stimulate ovarian function and regulate the menstrual cycle. Additionally, the adrenal glands secrete androgens and other hormones that influence reproductive health and are vital for libido and energy levels.
Issues with any of these glands can lead to common reproductive health disorders, including polycystic ovary syndrome (PCOS), ovarian cysts, and hormonal imbalances. Factors such as stress, diet, and lifestyle choices significantly impact gland health, affecting fertility and overall well-being. For instance, maintaining a healthy weight and managing stress through mindfulness or exercise can enhance hormonal balance and improve reproductive outcomes.
For many, understanding these glands’ functions and their interconnectedness demystifies the complexities of reproductive health. Regular health check-ups and being mindful of changes in one’s body can empower individuals to seek help promptly, paving the way for informed decisions about family-building paths, whether through natural conception, assisted reproductive technologies, or other options.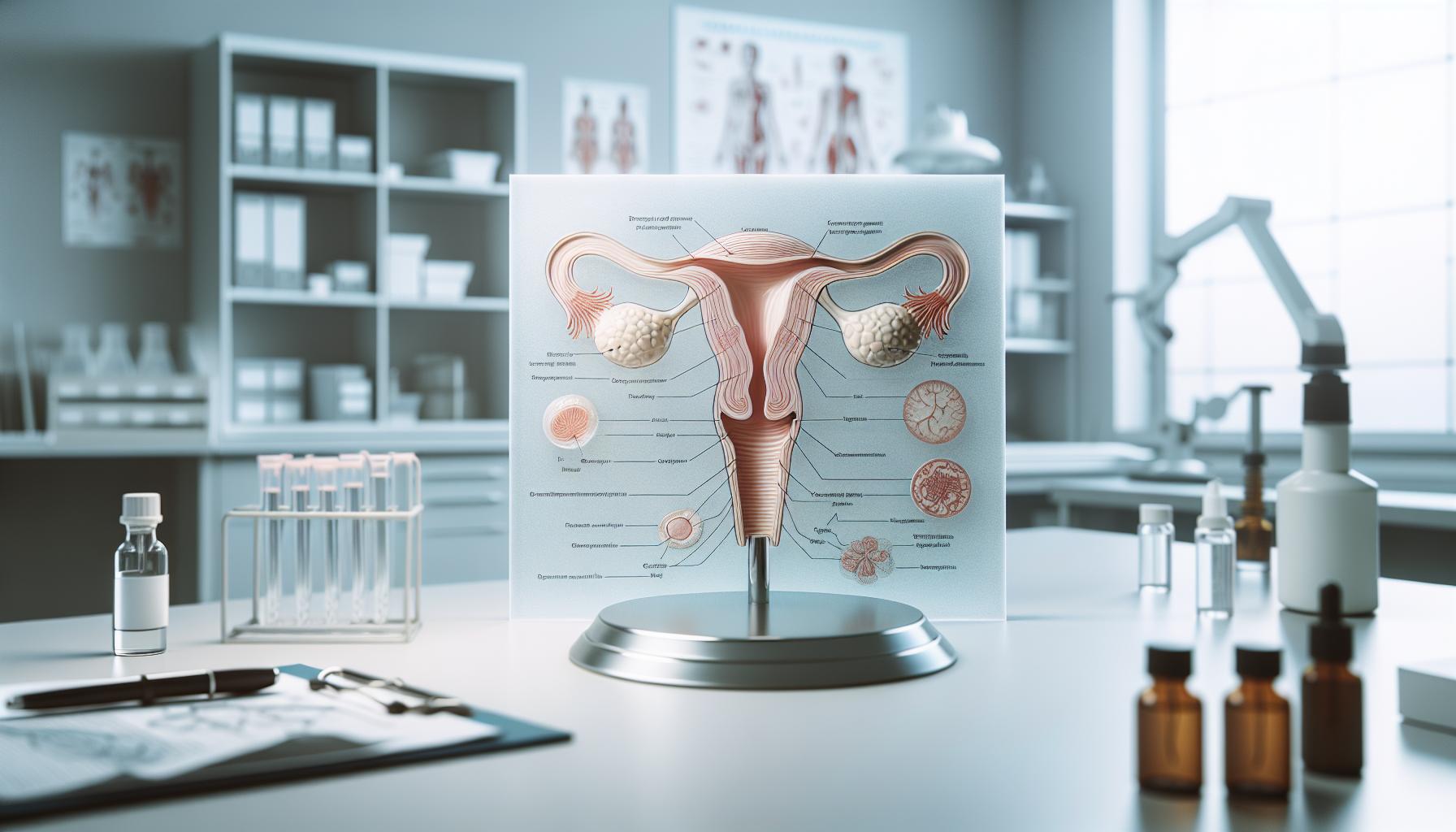
Anatomy of the Ovaries: Key Insights
The ovaries are remarkable structures that not only produce eggs but also play a crucial role in hormone production, shaping a woman’s reproductive health and overall wellness. Each ovary, approximately the size and shape of an almond, is located on either side of the uterus, connected by the fallopian tubes. Within these small organs lies the potential for life-thousands of immature eggs are stored within follicles, waiting for the right hormonal signals to mature and be released during the menstrual cycle.
In terms of their anatomy, the ovaries consist of two main sections: the outer cortex and the inner medulla. The cortex is where the follicles reside, while the medulla contains blood vessels and connective tissue. As women age, the number of follicles decreases, leading to changes in hormonal balance and eventually menopause, typically occurring between the ages of 45 and 55. This natural decline can signify various physical and emotional changes, but understanding ovarian health can help navigate these transitions with greater confidence.
The hormonal function of the ovaries is significant. They produce estrogen and progesterone, hormones that regulate not only the menstrual cycle but also influence mood, bone health, and cardiovascular function. When the hormonal balance is disrupted, whether through conditions like polycystic ovary syndrome (PCOS) or thyroid diseases, it can lead to various reproductive issues. Women experiencing irregular cycles, mood swings, or physical discomfort may benefit from monitoring their ovarian health and consulting healthcare providers for proper evaluation and guidance.
Understanding the anatomy of the ovaries is more than just an academic exercise; it’s about empowerment. Knowledge of how these glands function, the significance of their hormones, and the potential challenges can help individuals make informed decisions about their reproductive health. Whether considering family planning or seeking to understand hormonal changes, being attuned to what happens within the ovaries allows for a more proactive approach to health and wellness.
The Role of the Fallopian Tubes in Fertility
The fallopian tubes, often overlooked in discussions about fertility, play a pivotal role in a woman’s reproductive journey. These slender structures serve as conduits between the ovaries and the uterus, where fertilization occurs, making them vital to conception. Measuring approximately four to six inches in length, each tube extends from an ovary to the uterus, featuring the fimbriae-small, finger-like projections that help guide the egg from the ovary after ovulation.
Understanding the functionality of the fallopian tubes can demystify the process of conception for many. Once an egg is released from the ovary, it must travel through the fallopian tube, where it may encounter sperm that has journeyed from the uterus. Successful fertilization occurs when a sperm penetrates the egg, forming a zygote, which continues along the tube towards the uterus for implantation. If the tubes are blocked or damaged due to conditions such as endometriosis or pelvic inflammatory disease, it can prevent this crucial process, leading to infertility. Recognizing these potential barriers enables individuals and couples to seek appropriate evaluation and treatment options.
The health of fallopian tubes is often assessed through various diagnostic tests, including hysterosalpingography (HSG) or laparoscopy. These procedures can reveal blockages or abnormalities that may hinder fertility. For those facing challenges, treatments are available to help restore function or facilitate conception, such as in vitro fertilization (IVF), where fertilization occurs outside the body and the resulting embryo is implanted directly into the uterus.
In acknowledging the emotional weight of the fertility journey, it’s essential to approach these discussions with empathy and support. Many individuals may experience a range of feelings, from hope to frustration, and it’s important to validate those emotions. Resources and support networks are available to help navigate the complexities of reproductive health, ensuring that each person’s path-whether through medical intervention, adoption, or other family-building options-is respected and celebrated. Remember, understanding the role of your body’s systems, including the fallopian tubes, is an empowering step in your fertility journey.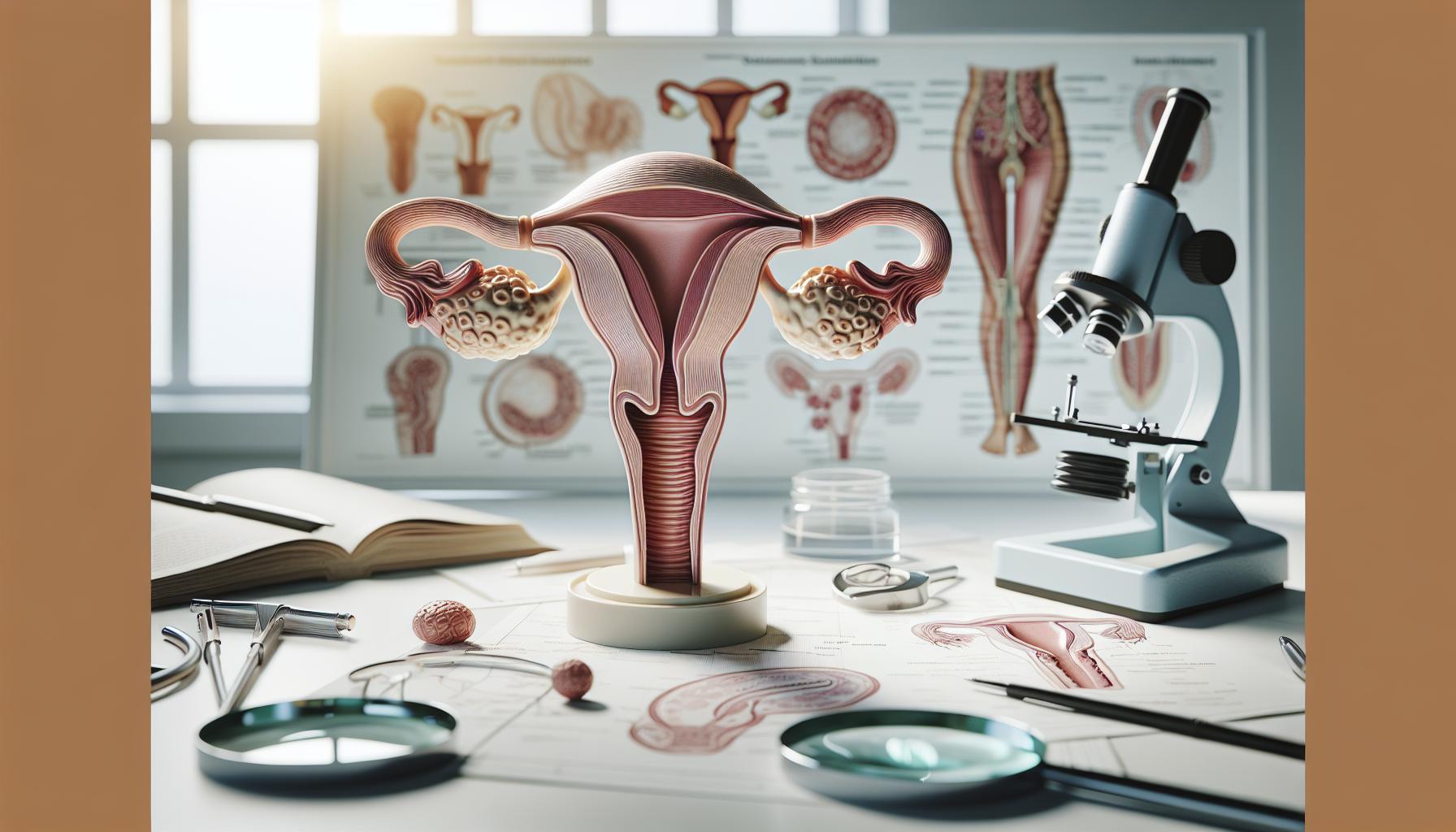
Exploring the Uterus: Structure and Function
The uterus, often referred to as the womb, is a remarkable and dynamic organ that plays a critical role in the female reproductive system. This pear-shaped structure not only houses a developing fetus during pregnancy but also serves key functions in the menstrual cycle and overall reproductive health. Understanding its anatomy and function can provide deeper insights into your fertility journey.
Structure of the Uterus
The uterus is situated in the pelvis, between the bladder and the rectum, and is supported by various ligaments that keep it in place. It consists of three main parts: the body, the fundus, and the cervix. The body is the largest section, where the fetus develops, while the fundus is the top rounded portion. The cervix, which opens into the vagina, plays a crucial role during childbirth by dilating to allow passage of the baby.
The uterine wall has three layers:
- Perimetrium: The outermost layer, providing a protective covering.
- Myometrium: The middle muscular layer, responsible for contractions during labor.
- Endometrium: The inner lining that thickens and sheds during the menstrual cycle, crucial for implantation of a fertilized egg.
Function of the Uterus
The primary functions of the uterus include facilitating menstruation, providing an environment for fertilization and fetal development, and playing a role in childbirth. During the menstrual cycle, the endometrium undergoes cyclical changes, thickening to prepare for a potential pregnancy. If fertilization does not occur, this lining is shed during menstruation.
In cases of pregnancy, the uterus adapts to accommodate the growing fetus, expanding significantly and providing nourishment and protection. The myometrium contracts during labor, helping to deliver the baby. Understanding this process can ease anxiety and emotional weight for those navigating fertility challenges.
It’s important to recognize that issues such as fibroids, endometriosis, or other disorders can affect uterine health, leading to complications in fertility. Regular monitoring and discussions with healthcare providers can help address concerns and guide you on proactive measures to maintain uterine health.
The journey of fertility can be laden with complex emotions, from excitement to disappointment. Validating these feelings is crucial, whether you are considering various family-building options or facing health challenges. Resources are available to support you through this journey, ensuring you feel empowered and informed every step of the way.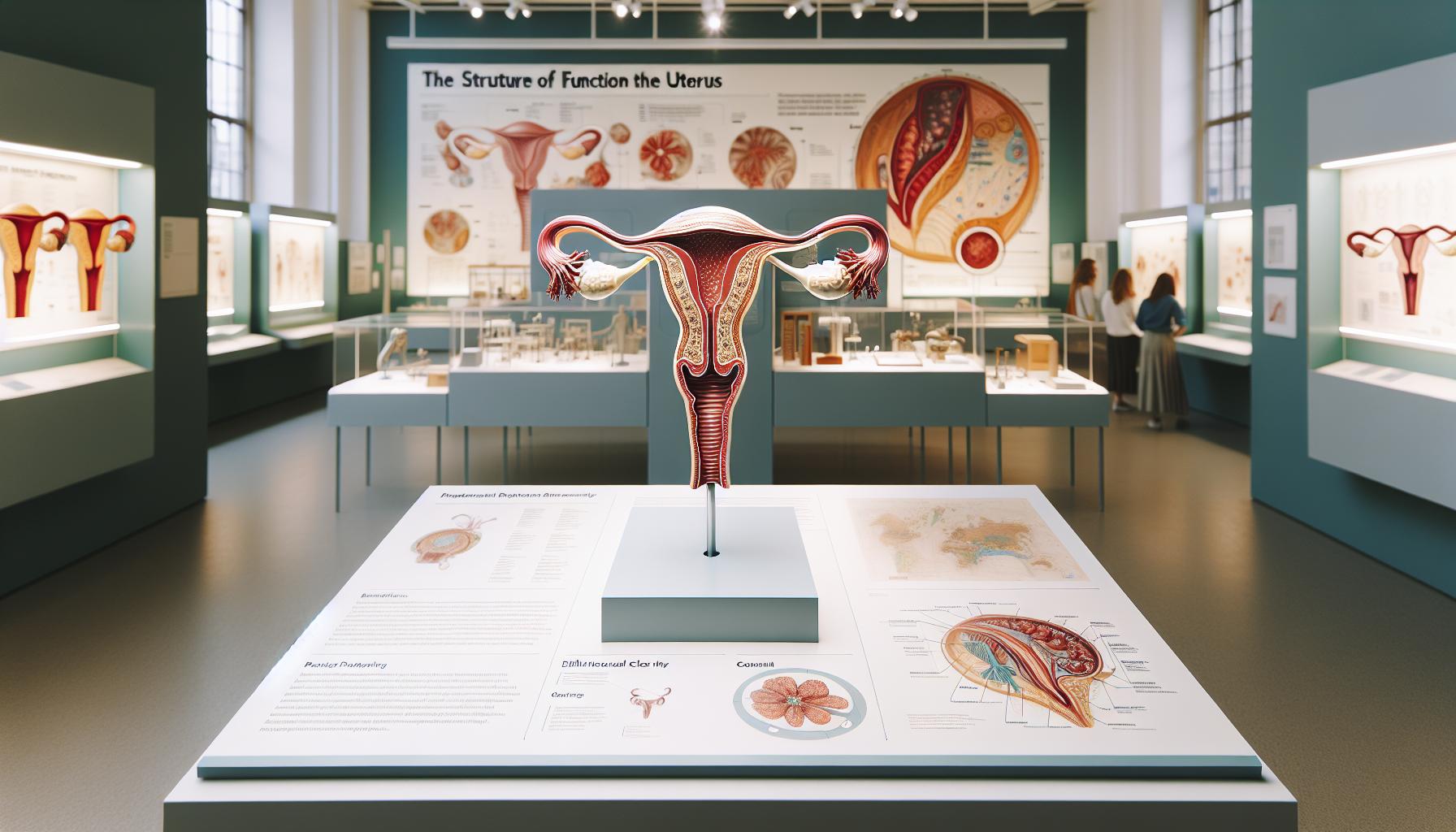
The Importance of the Endometrium in Reproduction
The endometrium plays a vital role in female reproduction, acting as the inner lining of the uterus where the crucial events of conception and implantation unfold. Each menstrual cycle, this tissue undergoes significant transformations in preparation for a potential pregnancy. If fertilization occurs, the endometrium thickens, creating a nurturing environment for the developing embryo. If not, it sheds during menstruation, making way for a new cycle. Understanding these processes not only illuminates the complexities of reproductive health but can also empower individuals on their fertility journeys.
The endometrial cycle is governed by hormonal changes primarily influenced by estrogen and progesterone. In the first half of the menstrual cycle, estrogen levels rise, leading to the proliferation of the endometrial cells, thereby thickening the lining in anticipation of an embryo. After ovulation, progesterone takes center stage, enhancing the endometrium’s capacity to support a fertilized egg. If no implantation occurs, these hormone levels drop, initiating the breakdown of the endometrium, culminating in menstruation. This cyclical nature of the endometrium highlights its responsiveness to hormonal signals and its critical role in reproductive health.
Common disorders of the endometrium, such as endometriosis or hyperplasia, can significantly impact fertility and overall health. Endometriosis, characterized by the presence of endometrial tissue outside the uterus, can cause pain and disrupt normal ovarian function. It’s essential for individuals experiencing symptoms like severe menstrual pain or irregular bleeding to consult a healthcare provider for thorough evaluation and potential treatment options. Early intervention can often lead to better outcomes and improved quality of life.
Caring for your reproductive health involves understanding how lifestyle factors affect the endometrium and overall fertility. Maintaining a balanced diet, managing stress levels, and avoiding smoking can positively influence hormonal balance and endometrial health. Additionally, regular check-ups with healthcare providers can facilitate the early detection of any issues, allowing for timely support and management. Navigating the emotional landscape of fertility can be challenging; it’s important to seek resources and support, whether through counseling or support groups, to help cope with the ups and downs of this journey. Remember, you are not alone, and there are many paths to explore in your pursuit of parenthood.
Hormonal Regulation of Female Reproductive Glands
The intricate dance of hormones is vital in regulating the female reproductive glands, influencing everything from menstrual cycles to fertility. Central to this orchestration are the ovaries, which produce essential hormones, primarily estrogen and progesterone. These hormones not only govern the development of follicles within the ovaries but also coordinate the timing of ovulation and prepare the endometrium for potential implantation of an embryo. For many, understanding this hormonal interplay can demystify the fertility journey and empower proactive health decisions.
In a typical menstrual cycle, the cycle begins with the hypothalamus releasing gonadotropin-releasing hormone (GnRH), prompting the pituitary gland to secrete follicle-stimulating hormone (FSH) and luteinizing hormone (LH). FSH stimulates ovarian follicles to mature, leading to the production of estrogen. As estrogen levels rise, they signal the pituitary gland to reduce FSH production while increasing LH secretion, culminating in ovulation. After this, the ruptured follicle transforms into the corpus luteum, which releases progesterone. If fertilization does not occur, the levels of estrogen and progesterone drop, leading to menstruation, marking a new cycle.
Understanding these hormonal levels is crucial for individuals experiencing difficulties with fertility or irregular cycles. Tracking these fluctuations can provide insight into ovulation patterns and potential issues. For instance, irregularities in hormone levels may indicate conditions such as polycystic ovary syndrome (PCOS) or thyroid issues, which can significantly impact reproductive health.
Support along the fertility journey is essential, as the emotional toll can be profound. It’s important to seek assistance from reproductive health specialists who can offer tailored advice and treatment options. Whether you’re considering assisted reproductive technologies or looking for support in understanding your body, remember that knowledge is empowering. Celebrate small milestones and take each step at your pace. Connecting with others who share similar experiences can also provide comfort and validation during this deeply personal journey.
Common Disorders of Female Reproductive Glands
Understanding the intricate relationships within the female reproductive system is key to recognizing and addressing potential disorders of the reproductive glands. Disorders can range from common conditions to more serious diseases, each presenting unique challenges and emotional impacts. Acknowledging these challenges and seeking proper support is vital for maintaining both physical and emotional health.
One of the most prevalent disorders affecting the female reproductive glands is Polycystic Ovary Syndrome (PCOS). This hormonal disorder is characterized by the presence of multiple cysts on the ovaries, irregular menstrual cycles, and elevated levels of androgens (male hormones). Women with PCOS may experience symptoms such as weight gain, acne, and fertility issues. Understanding PCOS is crucial for those affected, as lifestyle changes, hormonal interventions, and medications can significantly improve symptoms and fertility outcomes.
Another common condition is Endometriosis, where tissue similar to the lining inside the uterus grows outside of it, often causing severe pain, especially during menstruation. This condition can lead to complications such as fertility issues and chronic pelvic pain. Management often involves medication, lifestyle adjustments, or surgical options for those seeking relief from severe symptoms or attempting to enhance fertility.
Uterine fibroids are also a significant concern. These benign tumors can develop in the uterus and cause heavy periods, discomfort, and pressure symptoms. While many women may not require treatment, those with significant symptoms might explore options such as hormonal therapy or surgical removal. Awareness of these possibilities can empower individuals to discuss their symptoms openly with their healthcare providers.
In addition to these disorders, lifestyle factors such as diet, exercise, and stress management play a critical role in reproductive health. Regular physical activity and a balanced diet can positively impact hormonal balance and overall well-being, addressing some of the underlying issues that contribute to reproductive disorders.
Navigating these challenges can be emotionally taxing. It’s essential to validate feelings of hope, grief, and uncertainty. Whether considering assisted reproductive technologies, connecting with support groups, or simply seeking information, remember that you are not alone on this journey. Make space for small victories along the way, and don’t hesitate to reach out for the compassionate care and support you deserve.
Impact of Lifestyle on Reproductive Health
The connection between lifestyle choices and reproductive health is profound and far-reaching. Engaging in healthy behaviors not only enhances general well-being but significantly influences the functioning of the female reproductive glands. Simple changes can make a notable difference in hormonal balance, menstrual regularity, and overall fertility.
Regular physical activity is one of the most effective ways to boost reproductive health. Exercise helps regulate weight, improves blood circulation, and can balance hormones, all of which are critical for optimal ovarian function and fertility. Women who maintain a healthy weight and engage in consistent physical activity often experience more regular menstrual cycles and improved ovulation.
Nutrition also plays a vital role. A balanced diet rich in whole foods, vitamins, and minerals can support reproductive health in multiple ways. Foods high in antioxidants, such as fruits and vegetables, can combat oxidative stress, which is a factor in infertility. Additionally, incorporating healthy fats, such as those found in avocados and nuts, can help regulate hormones. It’s important to limit processed foods and sugars, as these can lead to hormonal imbalances.
Stress management cannot be overlooked in the discussion of lifestyle impacts on reproductive health. Chronic stress can disrupt the body’s hormonal equilibrium and lead to conditions such as PCOS or irregular menstrual cycles. Techniques such as mindfulness, yoga, and adequate sleep are crucial for reducing stress levels and promoting a healthier reproductive system.
Equally important is the consideration of environmental factors. Exposure to endocrine disruptors-chemicals found in some plastics and personal care products-can negatively impact hormonal health. Opting for natural products and reducing plastic use can be a simple yet effective way to safeguard reproductive health.
Finally, the emotional journey of trying to conceive often comes with challenges that go beyond physical health. Many women experience feelings of uncertainty or anxiety regarding fertility. Building a support system or seeking professional counseling can be beneficial for maintaining emotional well-being throughout the process.
In summary, lifestyle choices profoundly affect the female reproductive glands. By prioritizing a balanced diet, regular exercise, stress management, and minimizing exposure to harmful substances, women can optimize their reproductive health. Remember, small, consistent changes can lead to significant improvements over time, and it’s essential to celebrate every step on the journey towards reproductive wellness.
Tests and Procedures for Evaluating Gland Health
Understanding the health of the female reproductive glands is crucial for maintaining overall reproductive wellness. Various tests and procedures are available to evaluate gland health, often providing invaluable insights for women navigating their fertility journeys. These evaluations can help identify issues early, allowing for timely interventions and better management of reproductive health.
One of the foundational tests is the pelvic ultrasound, which uses sound waves to create images of the reproductive organs, including the ovaries and uterus. This non-invasive procedure can help detect conditions like ovarian cysts, fibroids, and abnormalities in the uterus that could impact fertility. Women often find this test straightforward, and it can usually be performed in an outpatient setting.
Blood tests play a significant role in assessing hormonal levels-key indicators of gland health. For instance, measuring Follicle-Stimulating Hormone (FSH) and Luteinizing Hormone (LH) can reveal insights into menstrual cycle regularity and ovarian function. Additionally, tests for Estrogen and Progesterone levels can inform healthcare providers about ovulation and overall hormonal balance. Understanding these levels is essential not only for diagnosing conditions, such as polycystic ovary syndrome (PCOS) but also for tailoring appropriate treatment strategies.
Another important procedure is hysterosalpingography (HSG), which involves injecting a dye into the uterus and fallopian tubes to ensure they are open and healthy. This test can help address concerns around infertility related to blocked tubes or uterine abnormalities. While some women may feel discomfort during the procedure, it can provide critical information that can guide future fertility treatments.
Lastly, it’s important to remember that evaluations go beyond just physical assessments. Many women experience emotional responses to these tests and procedures. Feelings of anxiety, fear, or uncertainty are completely normal and should be addressed openly with healthcare providers. Building a supportive network, whether through partners, friends, or community resources, can make a significant difference in navigating these evaluations and the subsequent medical journey.
In summary, tests and procedures for evaluating female reproductive gland health are essential tools that can uncover critical information about reproductive wellness. From ultrasounds to blood tests and beyond, these evaluations provide a clearer picture of fertility status and help guide women toward successful family-building paths.
Treatment Options for Reproductive Health Issues
When facing reproductive health issues, understanding your options can feel overwhelming, yet it is essential to know that many pathways can lead to improved fertility and reproductive wellness. Each treatment option is tailored to address specific concerns, ranging from hormonal imbalances to anatomical challenges, and aims to support your unique journey toward conception.
One of the most common approaches is medication therapy. Hormonal treatments, such as Clomiphene Citrate or Gonadotropins, can help stimulate ovulation in women with irregular cycles or conditions like PCOS. These medications typically cost between $50 to $100 per cycle, depending on insurance coverage. Monitoring through blood tests and ultrasounds is often involved to track the response, which may require multiple visits to your healthcare provider.
If medication alone does not yield desirable results, assisted reproductive technologies (ART) such as In Vitro Fertilization (IVF) may be recommended. IVF involves retrieving eggs and fertilizing them in a lab, followed by transferring one or more embryos into the uterus. The process can cost around $12,000 to $15,000 per cycle, with potential additional expenses for medications, genetic testing, and cryopreservation. While success rates vary based on age and health factors, many clinics report success rates of 40% to 50% for women under 35.
For couples facing male factor infertility, treatments such as Intrauterine Insemination (IUI) or Intracytoplasmic Sperm Injection (ICSI) may be suitable. IUI involves placing sperm directly into the uterus around the time of ovulation and typically costs $300 to $1,000 per cycle. ICSI, where a single sperm is injected into an egg, is often part of an IVF procedure and can significantly enhance fertilization rates, especially in cases of low sperm motility or count.
In addition to medical treatments, lifestyle adjustments are crucial. Maintaining a balanced diet, engaging in regular physical activity, and managing stress levels can enhance fertility. Supplements like folic acid and omega-3 fatty acids may also support reproductive health. It’s vital to discuss any changes with your healthcare provider, ensuring they align with your treatment plan.
Navigating this journey can evoke a mix of emotions, from hope to anxiety. Celebrate small milestones along the way, and remember that seeking support from friends, family, or counseling can be beneficial. Understanding that you are not alone and fostering a community around you can make a significant difference in managing the emotional toll of reproductive health challenges.
Navigating Emotional Aspects of Reproductive Health
Navigating the emotional landscape of reproductive health can often feel overwhelming and isolating. Many individuals face a myriad of feelings-hope, anxiety, grief, and uncertainty-especially when dealing with challenges on the journey to conception. Understanding that these emotions are valid and common is the first step toward fostering a supportive environment that encourages healing and personal growth.
One of the most significant emotional challenges arises from the unpredictability of fertility treatments. Procedures like In Vitro Fertilization (IVF), often expensive and complex, can result in a rollercoaster of emotions due to fluctuating success rates, which vary widely based on age and health factors. For instance, IVF success rates for women under 35 can hover around 40% to 50%, yet every cycle can carry with it hopes for a baby and the stress of potential disappointment. Being open about these experiences-not bottling them up-can pave the way for healing. Celebrate small milestones along this journey, whether that includes starting a new treatment, getting through a tough day, or simply finding moments of joy amidst uncertainty.
Support networks play a crucial role in navigating this emotional terrain. Connecting with others who are experiencing similar hurdles-whether through online forums, local support groups, or counseling services-can help lessen feelings of isolation. These spaces allow for shared stories, coping strategies, and emotional solace, reaffirming that you are not alone in this journey. It’s also essential to engage supportive friends and family, ensuring their understanding and willingness to listen without judgment.
Finally, consider the significance of self-care throughout this process. Prioritize activities that nurture emotional well-being, such as meditation, gentle exercise, or creative outlets like journaling or art. Create a routine that balances treatment plans with moments of joy, reflection, and relaxation. Navigating the emotional aspects of reproductive health is undeniably challenging, but acknowledging your feelings, seeking community support, and taking proactive steps toward self-care can transform your journey into one of resilience and hope.
Empowering Your Fertility Journey: Resources and Support
The path to understanding and navigating your fertility journey can often feel daunting, yet the availability of resources and support can make this journey more manageable and hopeful. One vital step is gaining access to trustworthy information tailored to women’s reproductive health, which empowers you with knowledge about your body, the functioning of female reproductive glands, and common conditions that may arise.
Start by connecting with healthcare professionals who specialize in reproductive health. A fertility specialist can provide comprehensive evaluations and personalized guidance tailored to your unique situation. This includes understanding the anatomy of your reproductive glands and how they interact throughout the fertility process. Seek out clinics that offer transparent information regarding treatment options, costs, and success rates. It’s essential to have a clear roadmap of potential courses of action, such as hormonal treatments or assisted reproductive technologies like IVF or IUI (Intrauterine Insemination).
Additionally, support networks can profoundly impact your emotional well-being. Engaging with local support groups or online communities allows you to share experiences and gain insights from others facing similar obstacles. Whether it’s through forums that focus on infertility, adoption, or alternative family-building paths, being part of a community can alleviate the feelings of isolation frequently experienced during this journey. Consider resources like counseling services that specialize in reproductive health, which can offer a safe space to address your emotional responses, validate your feelings, and explore coping mechanisms.
Lastly, focus on self-care practices that honor your emotional and physical needs. Activities like mindfulness meditation, yoga, or journaling can provide grounding during stressful periods. Remember to celebrate small milestones, whether they’re related to your treatment or personal achievements. Acknowledge your emotions and allow yourself the grace to navigate this journey at your own pace. With the right resources, support, and self-compassion, you can feel empowered on your fertility journey.
Frequently asked questions
Q: What are the key functions of the female reproductive glands?
A: The female reproductive glands, including the ovaries, produce hormones like estrogen and progesterone, and are crucial for ovulation and menstruation. They also play a role in sexual development, fertility, and the overall regulation of the menstrual cycle. Understanding these functions can enhance reproductive health insights.
Q: How do female reproductive glands affect hormone levels?
A: Female reproductive glands regulate hormone levels through a complex interplay of feedback mechanisms. The ovaries release hormones that influence the menstrual cycle and support pregnancy, making them vital for hormonal balance. For a deeper understanding, refer to the section on hormonal regulation in our article.
Q: What conditions can affect the health of female reproductive glands?
A: Various conditions such as polycystic ovary syndrome (PCOS), endometriosis, and ovarian cysts can impact the health of the female reproductive glands. These disorders may disrupt hormonal balance and fertility. Explore our section on common disorders for more details.
Q: When should women see a doctor regarding reproductive gland health?
A: Women should consult a doctor if they experience irregular menstrual cycles, severe pelvic pain, or abnormal bleeding. Early diagnosis can prevent complications related to reproductive gland health. For additional guidance, check out our section on tests and procedures.
Q: What lifestyle changes can support healthy female reproductive glands?
A: Maintaining a balanced diet, exercising regularly, managing stress, and avoiding smoking can significantly benefit the health of female reproductive glands. These changes promote hormonal balance and overall reproductive health-discover more in our lifestyle impact section.
Q: How does age impact the function of female reproductive glands?
A: Age affects the function of female reproductive glands, particularly as women approach menopause. Hormone production decreases, leading to changes in menstrual cycles and fertility. For comprehensive insights into this transition, refer to our article’s hormonal regulation section.
Q: What imaging tests are used to evaluate female reproductive glands?
A: Imaging tests such as ultrasounds and MRIs are commonly used to evaluate the health of female reproductive glands. These tests can detect abnormalities like cysts or tumors. For detailed information on procedures, see our dedicated section.
Q: Are there alternative therapies that support female reproductive health?
A: Yes, alternative therapies such as acupuncture, yoga, and herbal remedies may support female reproductive health. Always consult a healthcare professional before starting any new treatment. For more holistic approaches, consider visiting our resources page.
In Conclusion
Understanding the female reproductive glands is essential for recognizing their vital role in hormonal balance and reproductive health. By grasping how these glands function, you’re better equipped to address concerns about fertility or hormonal imbalances. If you’re facing challenges, remember you’re not alone-many find support through treatments like IVF or insemination. Don’t hesitate to explore our guides on fertility options and insights into common causes of infertility.
Looking for more information? Be sure to check out our detailed articles on hormonal health and fertility treatments. And if you have questions or need personalized advice, consider signing up for our newsletter or scheduling a consultation with one of our compassionate team members. Your journey towards understanding and enhancing your reproductive health is important, and we’re here to support you every step of the way. Share your thoughts in the comments below, and let’s keep the conversation going!





