Understanding the intricacies of the reproductive system is vital for anyone on the journey of family building. Did you know that around 1 in 6 people of reproductive age experience infertility? This statistic underscores the importance of familiarizing ourselves with reproductive health, as knowledge can empower you to make informed decisions about your body and your future. In this article, we will delve into the highlighted part of the reproductive system, shedding light on its functions and significance in fertility. Whether you’re exploring options like IVF or looking to understand the emotional weight of this journey, grasping the basics can provide clarity. Join us as we navigate this complex landscape together, offering support and guidance along the way.
Understanding the Reproductive System: An Overview
Every individual has a unique connection to their reproductive system, which plays a critical role not just in biology, but in personal identity and health. At its core, the reproductive system is designed to perform vital functions that enable the continuation of species through reproduction. It is essential to understand how these systems function, their biological processes, and the factors that can influence reproductive health.
The female reproductive system is an intricate network of organs, including the ovaries, fallopian tubes, uterus, and vagina. It operates cyclically, primarily governed by hormones such as estrogen and progesterone. This system not only facilitates menstruation but also provides the environment for fertilization and development of a fetus. The male reproductive system, comprising the testes, prostate, and penis, is equally complex. Its primary function revolves around the production of sperm and hormones, particularly testosterone, which influences libido, muscle mass, and fertility.
Understanding the reproductive system extends beyond anatomy and physiology; it encompasses the emotional and psychological aspects of reproduction. Individuals may encounter a variety of challenges along their reproductive journeys, including conditions like polycystic ovary syndrome (PCOS), endometriosis, or low sperm count. These disorders can significantly impact one’s ability to conceive or maintain a healthy pregnancy, necessitating comprehensive knowledge about their symptoms and treatment options.
Moreover, innovative treatments in reproductive health are continuously evolving, offering hope and alternatives for those facing fertility issues. Techniques like in-vitro fertilization (IVF) and assisted reproductive technologies (ART) have provided pathways for many who may struggle with traditional conception methods. As we navigate the complexities of reproductive health, it is vital to foster inclusive dialogue around family-building options, ensuring access to resources for all individuals, regardless of their background or circumstances. This holistic understanding of the reproductive system empowers people to make informed choices, celebrate milestones, and seek the support they need along the way.
Key Functions of the Female Reproductive System

The female reproductive system is an extraordinary and complex network that not only supports the biological process of reproduction but also plays a crucial role in a woman’s overall health and emotional well-being. At its core, this system includes key organs such as the ovaries, fallopian tubes, uterus, and vagina, each contributing essential functions that together create a harmonious environment for reproduction.
One of the primary functions of the ovaries is to produce eggs (oocytes) and hormones like estrogen and progesterone, which regulate the menstrual cycle and prepare the body for potential pregnancy. The fallopian tubes serve as the pathway for the egg to travel from the ovary to the uterus and are the site where fertilization typically occurs, marking a pivotal moment in the reproductive process. Once fertilization happens, the uterus becomes vital as it provides a nurturing space for the developing embryo. If pregnancy does not occur, the menstrual cycle culminates in the shedding of the uterine lining, a natural and vital process that marks the beginning of a new cycle.
Beyond these physiological functions, it’s important to acknowledge the emotional landscape that accompanies reproductive health. Many women who experience challenges such as irregular cycles, hormonal imbalances, or conditions like endometriosis find themselves navigating a mix of emotions-grief, frustration, and, at times, uncertainty about the future. Recognizing this emotional weight is essential, and seeking support through counseling, support groups, or healthcare providers can resonate deeply with those on a fertility journey.
In addition to emotional support, understanding the impact of nutrition and lifestyle on reproductive health is critical. A balanced diet rich in vitamins and minerals can bolster hormonal health and overall well-being, while regular check-ups can help monitor any changes in reproductive function. By fostering a holistic approach that integrates physical health, emotional resilience, and an informed understanding of the reproductive system, women can empower themselves on their reproductive journey, celebrating both milestones and navigating challenges without feeling alone.
Key Functions of the Male Reproductive System
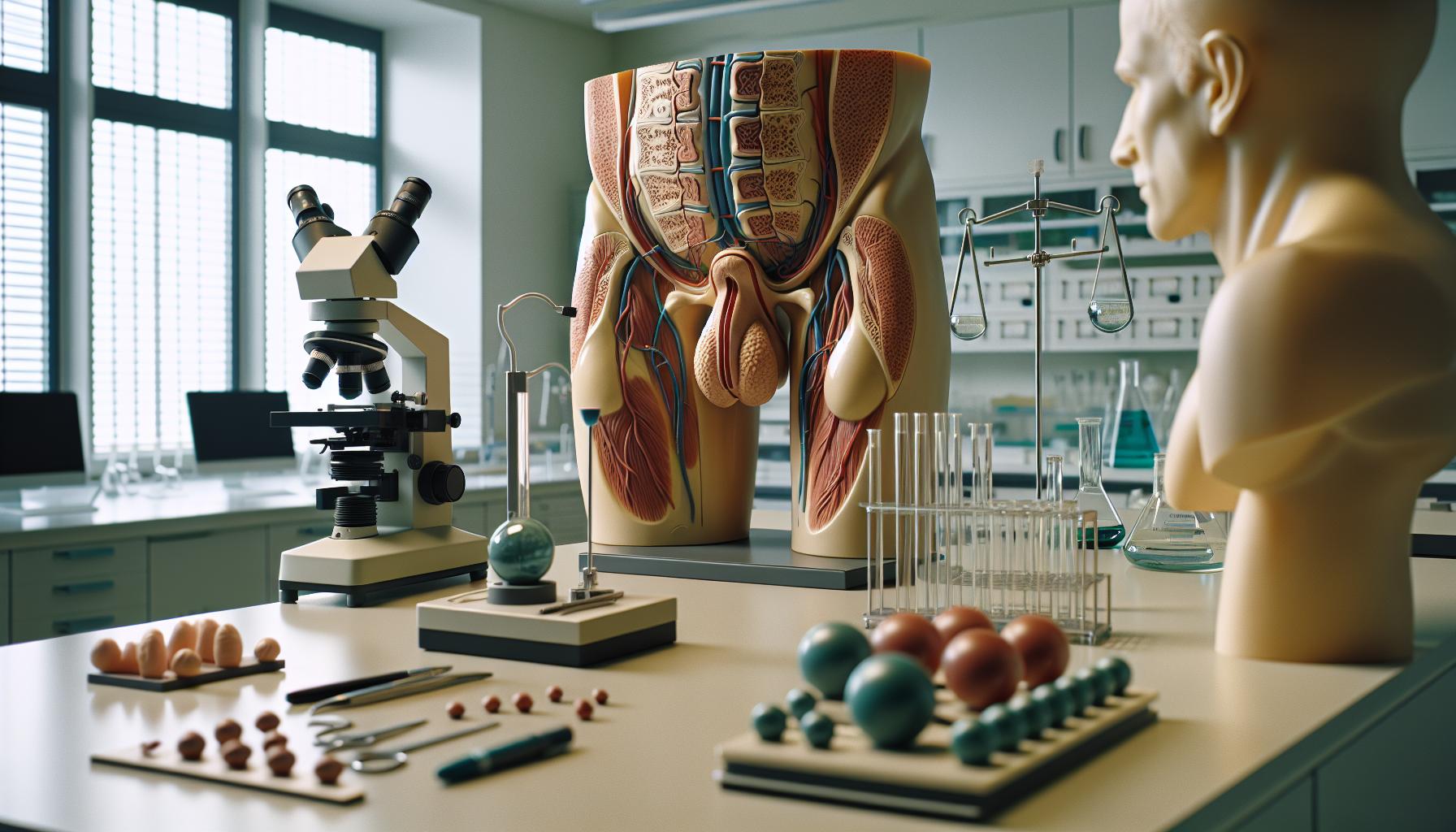
The male reproductive system is a complex network that plays a crucial role in the process of human reproduction. It not only facilitates the production of sperm but also produces hormones that are vital for overall health and reproductive function. Central to this system are the testes, which are responsible for sperm production and hormone secretion.
Spermatogenesis, the process of sperm production, occurs in the seminiferous tubules of the testes. This intricate process takes about 64 to 72 days and involves the transformation of spermatogonia into mature spermatozoa. Once sperm are produced, they are stored in the epididymis, where they undergo maturation and acquire the mobility necessary for successful fertilization. The vas deferens then transports mature sperm from the epididymis to the ejaculatory duct, where they mix with seminal fluid from various glands-such as the seminal vesicles and prostate-to form semen.
Hormones also play a key role in the male reproductive system. Testosterone, the principal male sex hormone, is produced in the testes and regulates several functions, including libido, energy levels, and the development of secondary sexual characteristics. The balance of these hormones is critical, as imbalances can lead to issues such as infertility, erectile dysfunction, or decreased libido.
Understanding these functions is essential not only for male reproductive health but also for maintaining overall well-being. Regular check-ups can help monitor reproductive health, and awareness of emotional challenges related to fertility and hormonal changes can provide crucial support for men navigating their own journeys. By celebrating milestones and seeking the right information, men can empower themselves in their reproductive health journey.
Common Disorders Affecting the Reproductive System
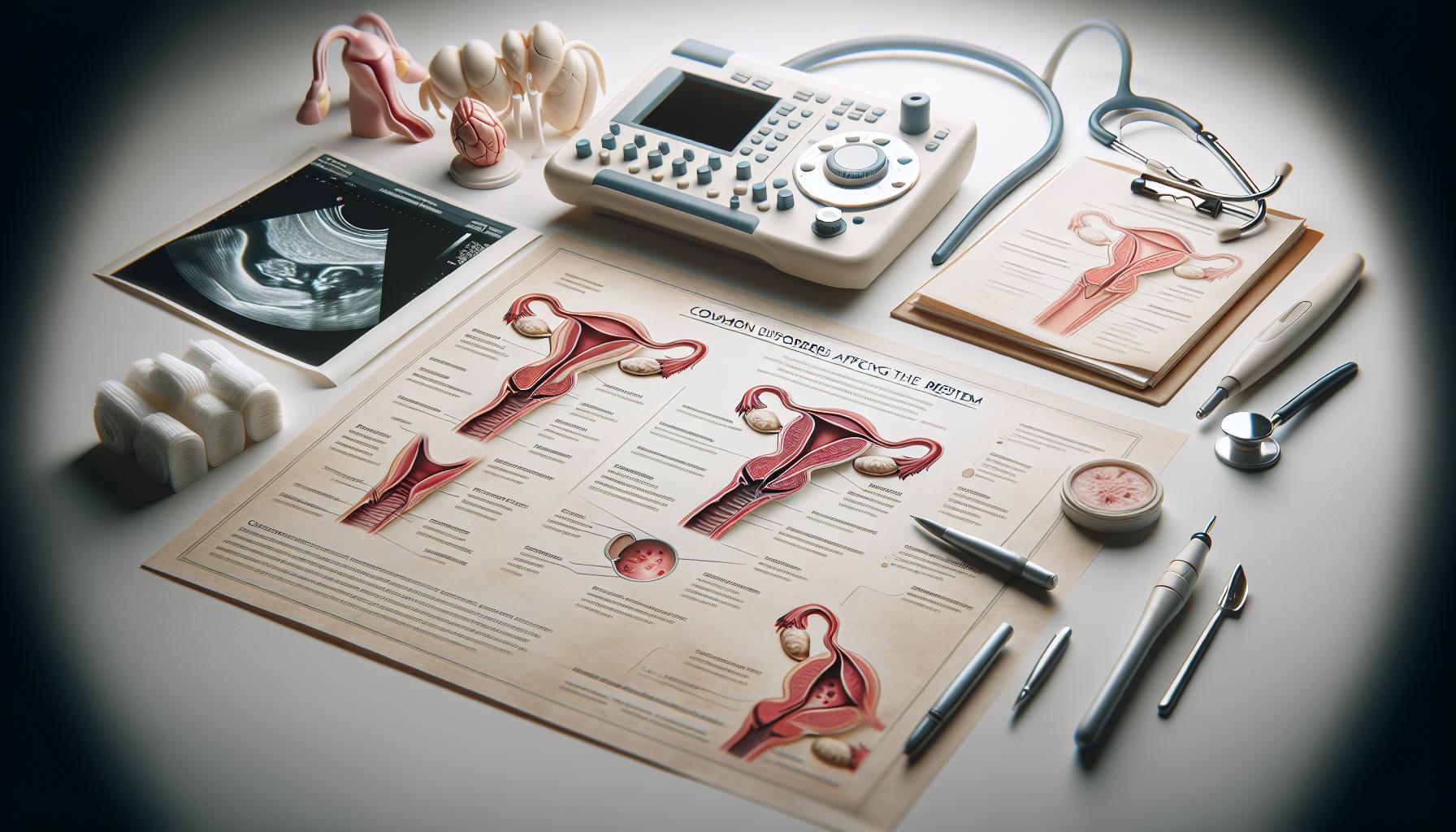
Many individuals may be unaware that disorders affecting the reproductive system can range widely from hormonal imbalances to structural anomalies, each carrying its own set of challenges and emotional burdens. One prevalent condition is polycystic ovary syndrome (PCOS), which affects about 1 in 10 women of reproductive age. PCOS can disrupt hormone levels, leading to irregular menstrual cycles, weight gain, acne, and fertility issues. Understanding and addressing these symptoms early on can empower those affected to seek suitable management options and improve their quality of life.
Common Disorders in Females
- Endometriosis: This painful condition involves the growth of endometrial-like tissue outside the uterus, which can cause severe pain, irregular bleeding, and fertility struggles. Treatment options include pain management, hormone therapy, and surgery in more severe cases.
- Uterine Fibroids: These benign tumors can significantly impact menstrual cycles and fertility. While some women may experience no symptoms, others may have heavy bleeding, discomfort, and complications during pregnancy. Treatment can range from monitoring to medication or surgery depending on severity.
The male reproductive system is not exempt from disorders either. Erectile dysfunction (ED) is a common issue that affects many men at various stages of life. Psychological factors, hormonal imbalances, or underlying health problems may contribute to ED, making it essential to assess and understand individual situations. Seeking professional advice can lead to effective treatment, which might include lifestyle changes, therapy, or medication.
Common Disorders in Males
- Low Testosterone: Also known as hypogonadism, this condition can lead to reduced libido, fatigue, and mood changes, affecting overall well-being and reproductive health.
- Varicocele: This condition refers to enlarged veins in the scrotum, which can negatively impact sperm production and quality, potentially contributing to infertility.
Being informed about these conditions is vital not only for identifying symptoms but also for understanding available options. Regular check-ups with healthcare providers can aid in the early detection of these issues, opening pathways to effective treatments and support. Each person’s journey through reproductive health is unique, and it is essential to acknowledge the emotional aspects involved-be it anxiety over fertility, the stresses of treatment processes, or the impact of financial constraints related to certain interventions like IVF or specialized surgeries. By prioritizing both physical and emotional health, individuals can build a supportive environment for themselves and their families, taking steps forward towards their reproductive goals.
Innovative Treatments in Reproductive Health

have made significant strides, offering hope to many individuals and couples facing fertility challenges. As technology advances, new methods emerge, allowing for personalized care tailored to individual needs. For example, in-vitro fertilization (IVF) has evolved beyond the traditional method, incorporating techniques such as preimplantation genetic testing (PGT) to detect genetic disorders before implantation, giving prospective parents more information on their options and reducing the chance of hereditary conditions.
The introduction of intrauterine insemination (IUI) is another key advancement, particularly for couples experiencing unexplained infertility. This procedure involves placing sperm directly in the uterus during ovulation, which has been shown to increase the likelihood of conception. Additionally, assisted reproductive technologies are now being combined with lifestyle interventions, such as nutritional guidance and stress management techniques, to enhance overall reproductive health outcomes.
For individuals with specific hormonal imbalances or conditions like PCOS, medical therapy has improved significantly. Medications such as clomiphene citrate or letrozole can stimulate ovulation more effectively than ever before. Furthermore, newer hormonal treatments aim to create a more favorable environment for conception and support overall reproductive health.
Emerging alternatives like egg freezing and sperm banking allow individuals to preserve their fertility for future family planning-especially beneficial for those facing health concerns or societal pressures that might delay childbearing. Understanding costs, success rates, and treatment timelines is essential; often, consultations with healthcare professionals can help demystify these options and provide clearer pathways to navigate emotional and financial aspects associated with treatment.
Each journey through reproductive health is unique, marked by its blend of challenges and opportunities. Therefore, seeking comprehensive care that respects personal circumstances is vital. It’s important to remember that while treatments offer hope, the emotional journey can be steep, and having supportive resources-whether through counseling, support groups, or community connections-plays an essential role in fostering resilience throughout this process.
The Role of Hormones in Reproduction
The intricate dance of hormones is essential for the successful operation of the reproductive system. Hormones such as estrogen, progesterone, and testosterone govern various processes, including the regulation of the menstrual cycle, ovulation, and sperm production. Each hormone plays a distinct role, and fluctuations in their levels can significantly impact fertility and overall reproductive health.
Key Hormones in Female Reproduction
In women, estrogen and progesterone are pivotal in preparing the body for potential pregnancy. Estrogen facilitates the thickening of the uterine lining, while progesterone stabilizes it after ovulation. If fertilization does not occur, hormone levels drop, leading to menstruation. Understanding these hormonal patterns can provide valuable insights for women trying to conceive, as monitoring may reveal optimal times for intercourse and help identify any irregularities that could affect fertility.
- Luteinizing Hormone (LH): Triggers ovulation and the release of eggs from the ovaries.
- Follicle-Stimulating Hormone (FSH): Stimulates the growth of ovarian follicles, essential for egg development.
- Prolactin: Involved in milk production and can affect menstrual cycles when present at abnormal levels.
Key Hormones in Male Reproduction
Testosterone is the primary male hormone, crucial for the development and maintenance of male reproductive tissues, as well as for the production of sperm. Levels of testosterone influence libido (sexual drive), mood, and energy levels, all of which can contribute to overall reproductive health.
- Luteinizing Hormone (LH): Stimulates testosterone production by the Leydig cells in the testes.
- Follicle-Stimulating Hormone (FSH): Essential for sperm production and maturation.
Navigating the complexities of hormonal balance can often feel overwhelming, especially for individuals and couples facing fertility challenges. It’s important to recognize that hormonal treatments, such as fertility medications, can help regulate these levels. Medications like clomiphene citrate for women or hormone replacement therapy for men can improve reproductive function when given under medical supervision. However, knowing what to expect during this journey is vital.
While hormonal treatments can provide hope and potential solutions, they may also bring about emotional fluctuations due to the underlying physiological changes. Understanding that these feelings are valid can be reassuring. Embracing a holistic approach that encompasses support systems-including counseling and community resources-can pave a clearer path through the emotional landscape of reproductive health.
In sum, hormones are the unseen architects of reproduction. Awareness of their influence can empower individuals on their fertility journeys, providing both practical tools for conception and empathetic acknowledgment of the emotional complexities at play.
Nutritional Impact on Reproductive Health
The food you eat can significantly impact your reproductive health, acting as both a foundation for fertility and a tool for enhancement during your family-building journey. Nutritional deficiencies or imbalances can hinder hormone production, impair ovulation, and affect sperm quality. Incorporating a balanced diet rich in essential nutrients not only supports these functions but also promotes overall well-being, which is crucial when navigating the emotional rollercoaster often associated with reproductive health challenges.
Key Nutrients for Reproductive Health
Aiming for a balanced intake of the right vitamins and minerals is crucial. Here are essential nutrients that play important roles in reproductive health:
- Folic Acid: Vital for women trying to conceive, folic acid helps prevent neural tube defects in developing embryos. Leafy greens, citrus fruits, and fortified cereals are excellent sources.
- Omega-3 Fatty Acids: These healthy fats, found in fish like salmon, flaxseeds, and walnuts, can improve hormone production and reduce inflammation, potentially enhancing fertility.
- Vitamin D: Low levels of this vitamin are linked to reproductive issues. Spending time in the sun and consuming foods like fatty fish and fortified dairy can help maintain adequate levels.
- Zinc: Important for testosterone production and sperm health in men, zinc-rich foods such as meat, shellfish, and legumes should be included in the diet.
Managing Weight and Lifestyle
Maintaining a healthy weight is instrumental in regulating reproductive hormones. Both underweight and overweight conditions can lead to irregular menstrual cycles and affect fertility. Engage in regular physical activity, as it not only aids in maintaining a healthy weight but also boosts mood and reduces stress, crucial elements when facing fertility challenges.
Furthermore, minimize processed foods and added sugars in your diet. These can spike insulin levels and lead to hormonal imbalances that may affect fertility. Instead, focus on whole, nutrient-dense foods that support your body’s needs.
Ultimately, a nutritious diet amplifies your body’s ability to cope with the emotional weight of the fertility journey. Establishing healthy eating habits can empower individuals and couples, creating a hopeful and proactive approach to reproductive health. Take small, mindful steps toward better nutrition, and remember that seeking support from a registered dietitian or fertility specialist can provide personalized guidance tailored to your unique needs.
Understanding Fertility: What You Need to Know
Understanding fertility involves recognizing the intricate dance of hormones, timing, and emotional well-being. Did you know that the window for conception is often shorter than many expect? In fact, a woman’s fertile window is typically just six days each menstrual cycle, culminating in ovulation when an egg is released from the ovaries. This brief period, combined with the lifespan of sperm-up to five days in a woman’s reproductive tract-necessitates timing and awareness for successful conception.
H3: The Role of Hormones in Fertility
Hormones play a pivotal role in regulating all stages of reproduction. In women, the menstrual cycle is orchestrated by a series of hormone fluctuations, including estrogen and progesterone. These hormones influence ovulation, preparing the uterine lining for a potential pregnancy. In men, hormones like testosterone and luteinizing hormone govern the production of sperm. Understanding these hormonal shifts can empower individuals to recognize their fertile days better, enhancing the chances of conception.
H3: Common Challenges and Solutions
Fertility can be affected by various factors, ranging from age and lifestyle to underlying health conditions. Conditions such as polycystic ovary syndrome (PCOS) in women or low testosterone levels in men can pose challenges. Lifestyle choices, including diet and exercise, also play a crucial role in reproductive health. Achieving a healthy weight and reducing stress through activities like yoga or meditation can create a more favorable environment for conception.
H3: Emotional Aspects of the Fertility Journey
Embarking on the journey towards parenthood can evoke a spectrum of emotions-hope, anxiety, grief, and sometimes frustration. It’s essential to acknowledge these feelings and seek support when needed. Connecting with others through support groups, whether in-person or online, can foster a sense of community and understanding. Remember, every individual’s journey is different, and celebrating small milestones can provide encouragement along the way.
Ultimately, understanding fertility is about recognizing the combination of biological, emotional, and practical elements that contribute to successful family-building efforts. Whether considering options like IVF, artificial insemination, or adoption, knowing the facts, setting realistic expectations, and advocating for one’s needs remain critical in navigating this deeply personal experience.
Navigating Emotional Challenges in Reproductive Health
Navigating the emotional landscape of reproductive health can be one of the most challenging aspects of the family-building journey. Whether you’re undergoing fertility treatments, dealing with pregnancy loss, or exploring alternative family-building options, it’s essential to acknowledge the depth of feelings that arise. From the soaring highs of hope to the heavy lows of grief, understanding that your emotions are valid can be a crucial first step in navigating this path.
Many individuals find immense comfort in connecting with others who share similar experiences. Joining support groups, both online and in person, can foster a sense of community and belonging. Here, you can share your journey, receive encouragement, and offer support to others. It’s not just about sharing struggles; celebrating small victories, like a positive pregnancy test or the first ultrasound, can weave a tapestry of shared joy and resilience. Remember, every journey is uniquely yours, and it’s perfectly okay to feel a mix of emotions as you move forward.
Consider carving out time for self-care practices that nourish not only your body but also your emotional health. Activities such as mindfulness meditation, journaling, or gentle exercise can help manage stress and anxiety. It’s also important to stay informed about your options-understanding the treatment process for methods like IVF or insemination can alleviate some uncertainties. Working with a mental health professional who specializes in reproductive health can provide tailored strategies and a safe space to process your feelings and experiences.
Lastly, be gentle with yourself. There may be days when hope feels distant and others when it surges unexpectedly. Recognizing this ebb and flow is part of the process. Allow yourself to grieve losses and to find joy in each step, however small. Engaging with a supportive community and prioritizing emotional well-being can make navigating the landscape of reproductive health not just manageable, but also a path toward connection and healing.
Inclusive Family-Building Options and Resources
Building a family is a deeply personal journey, and today there are more inclusive options than ever before. Whether you’re a same-sex couple, a single parent by choice, or facing medical challenges, knowing your family-building options can empower you on this path. The landscape of reproductive health is constantly evolving, offering several ways to create a family that aligns with your values and circumstances.
One of the most widely known options is in vitro fertilization (IVF), which has provided hope for many struggling with infertility. During IVF, eggs are retrieved and fertilized with sperm in a lab, and the resulting embryos are transferred to the uterus. Success rates can vary based on factors such as age, with younger individuals generally experiencing higher success rates. For those considering IVF, understanding the costs-which can range from $10,000 to $15,000 per cycle, not including medication-is essential for planning.
Another option is artificial insemination (AI), which is often less invasive and can be an effective route for both single parents and same-sex couples. Here, donor sperm is introduced into the reproductive tract during ovulation. Costs for AI can be significantly lower than IVF, generally around $300 to $1,000 per cycle, though pricing may vary based on donor selection and clinic fees.
Adoption presents yet another pathway to parenthood. It can be a fulfilling and meaningful way to build a family, although it comes with its own set of legal and emotional complexities. Costs associated with adoption can fluctuate widely based on whether you’re pursuing domestic, international, or foster care adoption. Some options may be subsidized through government programs, potentially easing financial burdens.
Understanding these options means acknowledging and preparing for the emotional highs and lows inherent in the journey. Community support is invaluable-online forums, local support groups, or counseling can provide comfort and connection as you navigate this emotional landscape. Celebrating milestones, no matter how small, can enhance your journey, reminding you of the joy amidst the challenges.
In this diverse world, it’s crucial to remember that no family looks the same. Consider reliable resources, such as fertility clinics that offer consultations, or organizations that focus on LGBTQ+ family-building. Each family-building story is unique, and having access to the right support can help you navigate this transformative chapter of your life successfully.
The Importance of Regular Health Check-Ups
Regular health check-ups are a cornerstone of maintaining reproductive health, acting as your first line of defense against potential issues. These visits provide an essential opportunity to monitor your body’s function and discuss any concerns regarding fertility or reproductive health. Detecting abnormalities early can significantly enhance your chances of successful treatment and remaining healthy.
During check-ups, healthcare providers typically conduct routine screenings-such as Pap smears for cervical health in women and testicular exams in men. These tests can identify conditions such as cervical cancer or testicular cancer at an early stage when they are most treatable. For individuals concerned about their fertility, regular assessments of hormone levels and reproductive organs can provide valuable insights into potential issues and guide treatment options effectively.
Understanding what to expect can alleviate some anxiety accompanying these appointments. In addition to physical examinations, discussions may cover menstrual cycles, sexual health, and lifestyle factors such as diet and exercise that directly influence reproductive health. It’s crucial to openly share any concerns with your healthcare provider-this can include anything from discomfort during menstruation to questions about your fertility timeline.
Lastly, approaching these appointments with a proactive mindset can be empowering. It’s an opportunity to not only gather information that may affect your health but also to build a supportive relationship with your healthcare provider. Remember, prioritizing your reproductive health through regular check-ups is not just about preventing problems-it’s about celebrating and maintaining your overall well-being.
Addressing Myths and Misconceptions About Reproduction
Unraveling the complexities of reproduction involves addressing the many myths and misconceptions that persist around this natural process. One common belief is that certain positions during intercourse can guarantee conception. In reality, while sperm can swim against gravity, there is no scientific evidence to suggest that specific sexual positions significantly boost the chances of getting pregnant. Instead, timing-understanding ovulation-is far more critical for enhancing fertility.
Another widespread myth is that female fertility dramatically declines and stops at a certain age. While it is true that fertility decreases as women age, particularly after 35, this decline is gradual and not an abrupt cutoff. Many women can conceive well into their late 30s or even early 40s, although the risks for pregnancy complications may increase. Hence, it’s essential to have personalized discussions with healthcare providers about fertility potential as one ages.
Men, too, are often subject to misconceptions regarding fertility. The belief that men can father children at any age is overly simplistic. Advanced paternal age has been linked to a range of issues in offspring, including genetic disorders. Furthermore, factors like lifestyle choices-such as smoking and alcohol consumption-can also affect sperm quality.
Addressing these beliefs is crucial for anyone on the reproductive journey. Understanding the realities of reproductive health allows individuals and couples to make informed choices, paving the way towards potential family-building options. Those struggling with fertility or seeking to expand their families are encouraged to seek information from reliable sources and engage in open dialogues with medical professionals. Embracing and debunking these myths can empower people, providing clarity and fostering a more supportive environment for their reproductive health journeys.
Q&A
Q: What are the main parts of the female reproductive system?
A: The main parts of the female reproductive system include the ovaries, fallopian tubes, uterus, and vagina. The ovaries produce eggs and hormones, while the fallopian tubes transport the eggs. The uterus is where a fertilized egg develops, and the vagina is the birth canal and the passage for menstrual fluid.
Q: What role do hormones play in the reproductive system?
A: Hormones such as estrogen and progesterone regulate the menstrual cycle, ovulation, and pregnancy. They are essential for developing sexual characteristics and preparing the body for potential conception. Hormone levels can impact overall reproductive health and function.
Q: How do reproductive disorders affect fertility?
A: Reproductive disorders, such as PCOS or endometriosis, can disrupt normal ovulation and hormonal balance, leading to challenges in conceiving. Early diagnosis and treatment can improve fertility outcomes and help manage symptoms effectively.
Q: What is the significance of regular health check-ups for reproductive health?
A: Regular check-ups are crucial for early detection of potential issues related to the reproductive system, such as infections or cancers. These visits can also provide guidance on reproductive health, family planning, and lifestyle choices that support well-being.
Q: How can diet impact the reproductive system?
A: A balanced diet rich in nutrients like folic acid, omega-3 fatty acids, and antioxidants supports reproductive health. Proper nutrition can enhance fertility, regulate menstrual cycles, and aid in the implementation of treatments like IVF.
Q: What are common myths about reproductive health?
A: Common myths include misconceptions about fertility age limits, the effectiveness of certain contraceptives, and the impact of lifestyle factors on reproductive capabilities. Educating oneself with reputable sources can help dispel these myths and promote informed decisions.
Q: What are some innovative treatments available in reproductive health?
A: Innovative treatments include IVF, IUI, and hormone therapy. These methods address various reproductive issues, helping couples conceive. New techniques, such as genetic screening and cryopreservation, improve success rates and allow for more personalized approaches to treatment.
Q: When should someone seek help for reproductive health issues?
A: Seek help if you experience irregular periods, severe pain, or difficulty conceiving after a year of trying. Early consultation with a healthcare provider can lead to effective management and treatment options tailored to your needs.
Insights and Conclusions
Understanding the reproductive system is crucial for anyone navigating fertility issues or family planning. By recognizing the highlighted parts of the reproductive system, you empower yourself with knowledge that can lead to informed decisions. If you’re curious to learn more about specific topics such as IVF, artificial insemination, or infertility causes, don’t hesitate to explore our comprehensive guides linked below.
Remember, this journey is personal and can feel overwhelming at times. Connect with us for expert insights, tools, and emotional support tailored to your needs. Join our community today, share your story, and let’s celebrate the milestones together. Don’t miss resources on navigating treatment costs and what to expect-your journey matters, and we’re here to walk alongside you.





