For many individuals, the choice to use an Intrauterine Device (IUD) as a long-term birth control method stems from its effectiveness and convenience. However, ongoing discussions about its potential effects on fertility can create uncertainty and concern among users. Understanding whether an IUD could influence future fertility is crucial for anyone contemplating their reproductive health. As we explore this important topic, we’ll address common worries and provide clarity on the relationship between IUDs and infertility. Navigating your fertility journey can be emotionally complex, and it’s essential to empower yourself with accurate information that respects your unique circumstances and future family-building aspirations. Let’s delve deeper into the facts, separating myths from realities, so you can feel confident in your choices moving forward.
Understanding IUDs and Their Purpose
Intrauterine devices (IUDs) have grown in popularity due to their effectiveness and convenience as a long-term birth control method. These small, T-shaped devices are inserted into the uterus to prevent pregnancy, providing a reliable option for women seeking to control their reproductive health. Understanding the purpose of IUDs can alleviate concerns, especially those surrounding their role in fertility.
IUDs serve primarily to prevent fertilization and implantation of an embryo. They work by creating an inhospitable environment for sperm and eggs through various mechanisms, including altering the uterine lining and thickening cervical mucus. This dual action helps ensure that pregnancy is not only avoided while the IUD is in place but also raises questions about their long-term effects on reproductive health, specifically regarding future fertility.
For many women, IUDs represent a proactive choice in family planning, allowing for flexibility and control over when or if they want to conceive. It’s vital to recognize that while some may worry about long-term fertility impacts, research indicates that once an IUD is removed, most women can return to their normal fertility levels relatively quickly. This transitional phase is often filled with hope and uncertainty, highlighting the importance of open conversations with healthcare providers to address any personal concerns or misconceptions.
Ultimately, the decision to use an IUD can be empowering, providing women the freedom to navigate their reproductive journeys at their own pace. While understanding that each person’s experience is unique, it is crucial to consider how this form of contraception aligns with individual family planning goals, ensuring that personal health choices are informed and respected.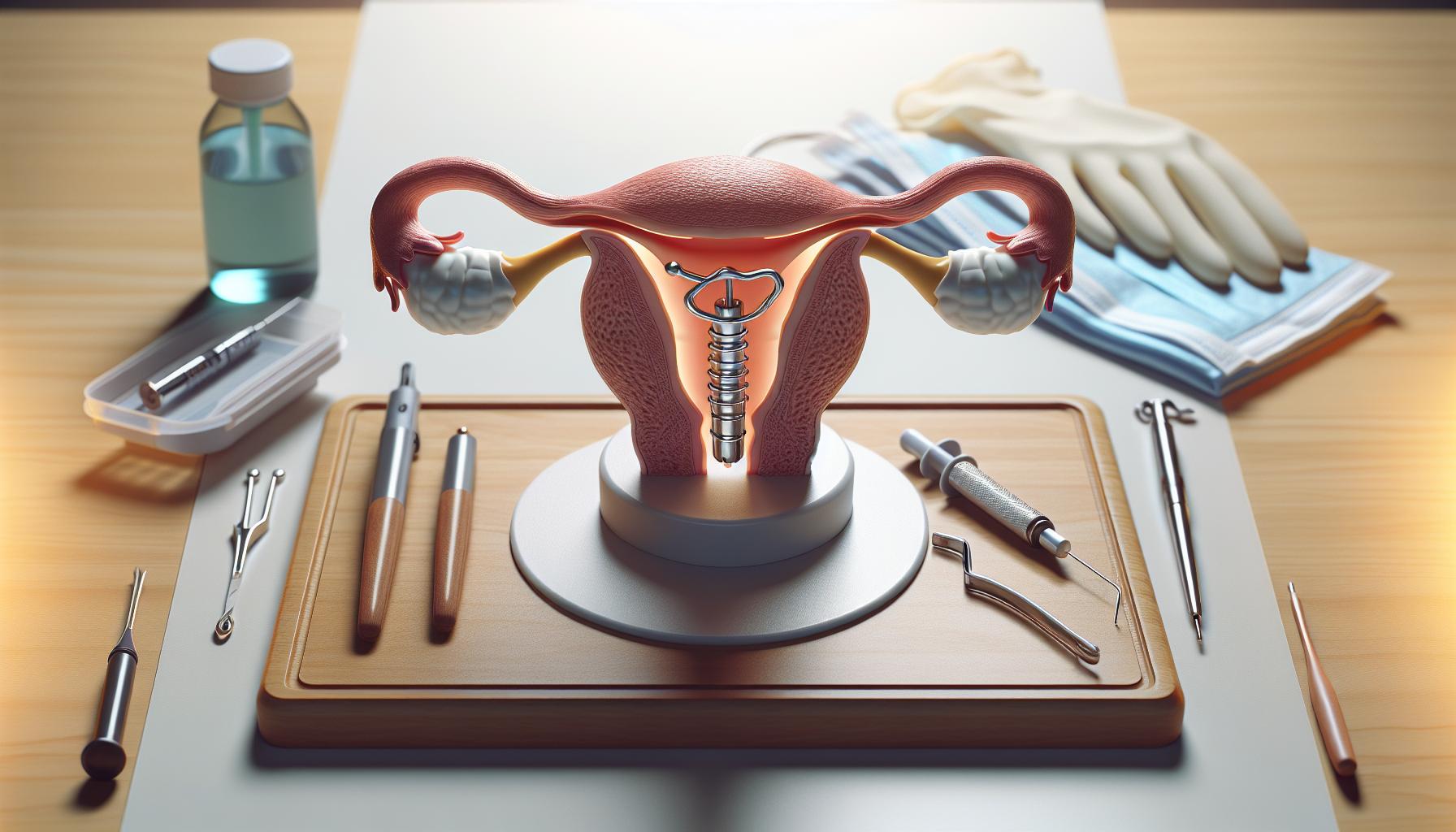
How IUDs Work: Mechanism of Action
IUDs, or intrauterine devices, are fascinating tools in the realm of contraception, offering women a reliable way to prevent pregnancy. They work primarily by creating a hostile environment for sperm, which inhibits fertilization and implantation. Understanding precisely how these devices function can alleviate concerns about their long-term effects on fertility and help demystify their use.
There are two main types of IUDs: hormonal and copper. Hormonal IUDs, such as Mirena and Kyleena, release progestin, a synthetic hormone that thickens cervical mucus, making it difficult for sperm to reach an egg. Additionally, they thin the uterine lining, reducing the chances of implantation if fertilization does occur. On the other hand, copper IUDs, like Paragard, utilize copper to create a toxic environment for sperm. The copper ions interfere with sperm motility and viability, while also causing an inflammatory reaction in the uterus that further prevents implantation.
While using an IUD is one of the most effective forms of birth control, it’s crucial to recognize that they do not protect against sexually transmitted infections (STIs). As a result, combining IUD use with barrier methods such as condoms enhances both pregnancy prevention and protection against STIs, adding an extra layer of safety during intimate encounters.
Many women wonder about the long-term implications of using an IUD, particularly regarding their future fertility. Research shows that once an IUD is removed, fertility typically returns to pre-IUD levels almost immediately for most users. This means that the device doesn’t cause permanent infertility. Understanding this can provide reassurance, allowing women to feel empowered in their family planning decisions, knowing they can frame their reproductive choices based on their lives and not out of fear of long-lasting effects from the IUD. It’s always advisable to discuss personal concerns during visits to healthcare providers, who can offer tailored support and guidance through the reproductive journey.
Common Misconceptions About IUDs and Infertility
Many women harbor concerns that using an IUD may lead to infertility, but this belief is often rooted in myths rather than scientific evidence. The reality is that research has consistently shown that IUDs do not affect a woman’s long-term fertility. In fact, once an IUD is removed, most women can expect their ability to conceive to return to baseline levels quite quickly. This immediate return of fertility can be empowering for those considering future family planning.
Among common misconceptions is the idea that IUDs somehow cause scarring or damage to the uterus, which in turn may lead to infertility. While it’s true that any medical procedure carries some risk, the insertion of an IUD is generally safe and well-tolerated. The primary purpose of an IUD is not only to prevent pregnancy but to do so in a reversible manner, allowing for full restoration of reproductive function upon removal. In particular, studies indicate that both hormonal and copper IUDs do not have lasting effects on the ovaries or the uterus that would impede a woman’s ability to conceive in the future.
It’s important to approach this topic with sensitivity, recognizing the emotional weight it can carry for many individuals. Concerns about fertility can often evoke feelings of anxiety and uncertainty, and misinformation can exacerbate these feelings. Open conversations with healthcare providers can alleviate fears and misconceptions. They can provide clear, evidence-based information about how IUDs function, the potential side effects, and the likelihood of returning to fertility after discontinuation. By understanding the facts, women can make informed decisions about their reproductive health and family planning goals.
The Science Behind IUDs and Fertility
The misconception that intrauterine devices (IUDs) lead to infertility persists despite ample research dispelling this myth. In fact, understanding the science behind how IUDs function can empower women and couples as they navigate their reproductive health. IUDs, whether hormonal or copper, work primarily by creating an environment that is inhospitable to sperm, thereby preventing fertilization. They do this without causing permanent changes to the uterus or ovaries, meaning that when an IUD is removed, fertility typically returns rapidly to baseline levels.
This quick rebound in fertility is supported by numerous studies indicating that the use of IUDs does not result in lasting damage or scarring of the uterine lining. In clinical settings, healthcare providers often reassure patients that both hormonal and copper IUDs do not interfere with ovulation or egg production. Instead, they primarily function by preventing sperm from reaching the egg or by altering the uterine lining to prevent implantation. For those concerned about potential long-term effects on fertility, it is crucial to recognize that the body often resumes its natural hormonal cycles immediately after IUD removal, with many women conceiving soon after.
It’s also important to address the emotional weight associated with fertility concerns. Many individuals experience anxiety when considering fertility and family planning, particularly when faced with mixed messages about contraceptive methods. Open, honest discussions with healthcare providers can help demystify the role of IUDs. Provider-patient relationships grounded in trust and communication can alleviate fears, allowing for a clearer understanding of personal reproductive health options. Those interested in family planning should feel empowered to seek guidance tailored to their unique circumstances, reinforcing that their reproductive choices will not permanently hinder their fertility.
Ultimately, navigating the complexities of birth control and fertility can feel overwhelming, but informed choices based on scientific evidence can foster confidence. Whether considering an IUD or exploring other family-building avenues, remember that there are supportive paths available, and it’s important to prioritize your well-being and peace of mind in the journey ahead.
Long-Term Effects of IUD Use on Reproductive Health
Despite lingering fears about the long-term effects of intrauterine devices (IUDs) on reproductive health, most research indicates that these contraceptives do not negatively impact fertility. When considering an IUD, many individuals wonder if it could affect their ability to conceive in the future. Understanding the evidence surrounding IUD use can provide clarity and reassurance during the family planning process.
The Impact of IUDs on Future Fertility
Studies show that both hormonal and copper IUDs are designed to prevent pregnancy without causing lasting changes to the uterine lining or ovarian function. The primary mechanism of action involves creating an environment that deters sperm from fertilizing an egg and preventing implantation. Once an IUD is removed, fertility typically rebounds quickly, usually within one to three menstrual cycles. This swift return to normalcy underscores that IUDs do not leave behind any permanent damage, making them a reliable option for those who plan to conceive later.
Addressing Emotional Concerns
It’s entirely normal to experience anxiety about fertility when using contraception. The fear of potential infertility can weigh heavily on individuals and couples, particularly when faced with conflicting information. It’s vital to foster open conversations with healthcare providers who can offer evidence-based guidance. Discussing your concerns can help in making informed choices that align with your reproductive goals.
Moreover, recognizing the spectrum of family-building options-such as IVF, adoption, or using assisted reproductive technology-can further enhance your confidence in the journey ahead. Remember that feeling ambivalent or uncertain about your choices is common; reaching out to supportive communities or professionals can help you navigate these feelings without judgment.
Conclusion
In reflecting on long-term IUD use, it’s important to prioritize your health and emotional well-being. Many women who have used IUDs report feeling empowered about their fertility choices and family planning, often conceiving shortly after removal. Each person’s journey is unique, and understanding the role of IUDs in your reproductive health can foster confidence and peace of mind as you move forward in your family planning journey.
Expert Insights: IUD Use and Future Fertility
Many individuals using intrauterine devices (IUDs) may find themselves grappling with questions about how their use could impact future fertility. It’s imperative to realize that not only do IUDs provide highly effective birth control, but extensive research indicates they do not have lasting effects on fertility once removed. The primary action of IUDs-whether hormonal or copper-works by creating an inhospitable environment for sperm and preventing fertilization and implantation. This mode of action allows for a quick recovery of fertility after the IUD’s removal, typically within one to three menstrual cycles.
Understanding the nuances of IUD usage and its implications on future fertility can alleviate many concerns. It’s common for individuals to feel anxious about the potential for infertility, particularly with the myriad of information available today. Engaging in conversations with healthcare providers can be incredibly beneficial, offering personalized insights and reassurance backed by scientific evidence. A supportive approach fosters open dialogue about your reproductive goals and any fears you may have without judgment.
Moreover, it’s essential to recognize that the journey toward family planning can encompass various paths. Options such as in vitro fertilization (IVF) or adoption can be part of your family-building strategy, and knowing this can help ease the emotional burden that uncertainties about fertility can bring. Celebrating small milestones along the way-such as having regular menstrual cycles post-removal-can help maintain a hopeful perspective as you navigate this journey. Remember, your feelings are valid, and seeking support from communities or professionals who understand your experience can make a significant difference.
Comparing IUDs with Other Birth Control Methods
Choosing the right birth control can evoke a whirlwind of emotions, especially when considering long-term fertility impacts. IUDs, or intrauterine devices, stand out as an effective option among various methods available today. They offer unique benefits compared to other contraceptive options like pills, implants, and condoms, which can help in making an informed decision.
To begin with, IUDs are often favored for their efficacy: both hormonal and copper IUDs boast a success rate of over 99% in preventing pregnancy. In contrast, combined oral contraceptive pills can be less effective if not taken consistently at the same time each day. For many, the long-term placement of an IUD-ranging from 3 to 10 years, depending on the type-provides peace of mind and removes the daily responsibility that comes with pills.
When comparing the side effects, it’s essential to consider individual health circumstances. Hormonal IUDs may lead to lighter periods or even amenorrhea (absence of menstruation), which can be appealing for those who struggle with heavy menstrual bleeding. On the other hand, some individuals may experience side effects such as mood changes or acne. Other methods like hormonal implants also share similar side effects but are effective for up to three years.
Furthermore, the emotional aspect of choosing contraceptive methods shouldn’t be overlooked. Condoms and other barrier methods, while offering the added benefit of protection against sexually transmitted infections (STIs), require consistent use and can sometimes disrupt intimacy. Recognizing the need for an accessible, effective method that aligns with personal lifestyle and health goals is crucial.
Ultimately, having a robust discussion with a healthcare provider can clarify options, tailor a solution to individual needs, and reassure those worried about long-term implications on fertility. Understanding both the functionality and emotional ramifications of these choices can foster an empowered approach to family planning, preparing for the journey ahead with confidence and support.
Addressing IUD Removal: What to Expect
The process of removing an intrauterine device (IUD) can be just as important as the decision to have one placed. Understanding what to expect can help ease any anxieties and prepare you for the experience, especially for those concerned about long-term fertility implications. Removal is generally a straightforward procedure, often taking less than a few minutes, and most individuals describe it as less uncomfortable than the insertion process.
When you visit your healthcare provider for IUD removal, they will first check the strings of the IUD to ensure they are in place. If the strings are not visible, further examination may be needed. The removal involves gently pulling on the strings to extract the device. In some cases, you might experience mild cramping or discomfort comparable to menstrual cramps during the procedure. Be assured that many find this experience manageable, and it may also be helpful to communicate any concerns with your provider beforehand to address them directly.
After the IUD is removed, it’s common to have bleeding or spotting. This can vary from person to person, and while some may notice heavier bleeding, others might not experience any bleeding at all. It’s essential to keep track of your body’s responses post-removal. If you have any significant concerns, such as severe pain or heavy bleeding that persists, reaching out to your healthcare provider is crucial.
For those considering future fertility, it’s heartening to note that IUD removal typically does not have long-term effects on fertility. Most people are able to conceive shortly after removal if they choose to do so. Still, it’s natural to have questions or worries about how this might affect your reproductive health. Engaging in an open dialogue with your healthcare provider can help clarify these questions, ensuring you feel confident in your family planning choices moving forward.
Personal Stories: IUD Experiences and Fertility
Many individuals who have used IUDs share a common concern about the long-term effects of these contraceptive devices on fertility. One woman, Sarah, felt a wave of relief when her doctor assured her that there is no evidence linking IUD use to infertility. After having the Mirena for five years, she was nervous about her ability to conceive once it was removed. However, when the time came, she and her partner were thrilled to discover they conceived within just a couple of months.
Another story comes from Mark, whose partner had varying experiences with her IUD; while it effectively prevented pregnancy, she often wondered how it might impact their future family plans. After doing thorough research together and speaking with healthcare providers, they learned that many people successfully conceive shortly after IUD removal. This knowledge gave them confidence as they decided to start trying for a baby.
Yet, not every journey is straightforward. Emily’s experience was filled with uncertainty. After having her IUD removed, she struggled to conceive for over a year. It was a tough emotional journey, marked by fluctuating hopefulness and disappointment. After consulting with a fertility specialist, they uncovered that the delay wasn’t connected to her previous use of an IUD. With a diagnosis of unexplained infertility, they explored a variety of options together. The process was daunting, but it emphasized the importance of open communication with healthcare providers.
These narratives highlight an essential truth: the emotional weight of reproductive choices can be heavy, filled with hope and uncertainty. Engaging with stories of others can foster a supportive community and validate feelings that many face during their fertility journeys, especially when navigating the complexities of birth control and future family planning. Remember that each experience is unique, and maintaining dialogue with healthcare providers is crucial to finding informed and compassionate solutions tailored to individual paths.
Infertility and IUDs: Medical Opinions and Research
Despite widespread concerns, the current medical consensus indicates that intrauterine devices (IUDs) do not cause infertility. Various studies have shown that the removal of an IUD typically leads to a nearly immediate return to fertility, allowing many women to conceive soon after discontinuation. Understanding the underlying mechanisms can provide reassurance to those contemplating the use of IUDs or those already using them.
Research suggests that while IUDs may temporarily affect the micro-environment of the uterus-such as altering the endometrial lining-they do not cause long-term damage or changes that would inhibit a woman’s ability to conceive. The likelihood of conception after IUD removal is high. In fact, one study indicates that approximately 80% of women who wished to conceive were able to do so within one year after removing the device. This perspective is crucial as many individuals operate under the misconception that IUDs can create lasting barriers to fertility.
Common Concerns and Reassurances
Many patients express fear that IUD use could contribute to complications such as ectopic pregnancies or chronic infertility. However, reputable sources emphasize that IUDs are actually associated with a lower risk of ectopic pregnancies compared to non-users. Additionally, the accommodations provided by IUDs-such as the reduction of heavy menstrual bleeding-can complement family planning by allowing for healthier reproductive cycles.
Ultimately, if concerns about future fertility arise, consulting a healthcare provider equipped with the latest research is essential. Open discussions can demystify feelings of anxiety about reproductive health and future family planning. Healthcare professionals are well-equipped to guide these conversations, helping to differentiate between fact and myth.
In conclusion, the ongoing dialogue in reproductive health emphasizes that while individual experiences may vary, the empirical evidence largely supports the safety of IUDs concerning fertility. Women should feel empowered to make informed decisions about their contraceptive options without the fear of long-term consequences on their future ability to conceive.
Navigating Concerns: When to Consult a Healthcare Provider
It’s completely normal to feel apprehensive about your reproductive health, especially when considering the potential implications of an IUD on future fertility. Many individuals find themselves grappling with concerns related to contraception, and understanding when to consult a healthcare provider can empower you along your journey. If you’ve been using an IUD and have questions – whether about its effects on fertility or your overall reproductive health – seeking the perspective of a knowledgeable provider can provide the clarity you need.
When to Reach Out
Consider consulting a healthcare professional in the following situations:
- Persistent Pain or Discomfort: If you experience ongoing pain, cramping, or unusual bleeding after IUD insertion, it could indicate an issue that warrants medical attention.
- Planning to Conceive: If you’re planning to get pregnant soon after IUD removal, discussing your plans with a healthcare provider can help ensure your body is ready for conception.
- Menstrual Changes: Noticeable changes in your menstrual cycle, such as heavier bleeding or missed periods, merit a discussion with your healthcare provider to rule out any complications.
- Concerns About Fertility: If you’re worried about how your IUD might affect your ability to conceive in the future, a healthcare provider can help dispel myths and provide accurate information.
Reaching out doesn’t have to wait until issues arise, either. Regular check-ups and open communication about your reproductive health can vastly enhance your understanding and facilitate a healthy dialogue around your options. Providers are equipped not only to assess your physical health but also to address emotional aspects, gently guiding you through any uncertainties regarding future family planning.
(h3) Embracing Your Options
Ultimately, knowledge is power. Remember, discussing your concerns with a healthcare provider can be a supportive step towards feeling more in control of your reproductive journey. They can help contextualize your experiences and provide tailored advice, whether your path leads to natural conception, assisted reproductive technologies, or alternative family-building options. You’re not alone in navigating these complex feelings – let your healthcare provider support you as you shape a future filled with your chosen possibilities.Empowering Choices: Family Planning with Confidence
Navigating the complexities of family planning can feel daunting, especially when weighing the options available to you, including the potential impacts of birth control methods like the IUD. One of the most common concerns among those considering or using an IUD is the worry about its impact on future fertility. It’s important to understand that while our reproductive journeys are personal and often influenced by many factors, the evidence supports that IUDs generally do not cause infertility.
The IUD, whether hormonal or copper, works by creating an environment in the uterus that is inhospitable to sperm, thereby preventing pregnancy. Importantly, once an IUD is removed, fertility typically returns to baseline levels almost immediately for most individuals. This means that if you decide to conceive after removing your IUD, the chances of becoming pregnant are generally unaffected by previous IUD use. Still, it’s crucial to communicate with your healthcare provider about your family planning goals, as they can provide tailored advice and support based on your specific situation.
Acknowledge the emotions tied to family planning decisions. It’s perfectly normal to feel a mix of hope and anxiety regarding your reproductive health and future pregnancies. Small milestones, like the decision to explore your options, should be celebrated, as they reflect your agency in your family-building journey. Remember that you are not alone-many individuals share similar concerns, and reaching out for support can provide reassurance.
Consider also the importance of educating yourself about everything from conception timelines post-IUD removal to understanding fertility treatments if needed. Embracing your options with confidence means being informed and proactive, whether that involves planning a timeline for conception, exploring assisted reproductive technologies like IVF, or discussing other paths such as adoption. Whatever your choices may be, having open conversations with your healthcare provider can empower you to move forward with a sense of control and clarity about your reproductive health.
Q&A
Q: Can IUDs lead to long-term fertility issues?
A: No, most research indicates that IUDs do not cause long-term fertility problems. After removal, most women can conceive normally. If you have concerns about your future fertility, consult your healthcare provider for personalized advice. Explore more in our section on Long-Term Effects of IUD Use on Reproductive Health.
Q: How long does it take to regain fertility after removing an IUD?
A: Fertility typically returns almost immediately after IUD removal. Most women can conceive within the first cycle following removal. If you’re planning a pregnancy, monitor your cycle and discuss any concerns with your provider, as covered in Expert Insights: IUD Use and Future Fertility.
Q: Are there specific medical conditions that make IUDs risky?
A: Yes, certain conditions, like pelvic inflammatory disease or certain uterine abnormalities, may increase risks associated with IUD use. If you have these conditions, consult your healthcare provider to discuss safe birth control options, as emphasized in Navigating Concerns: When to Consult a Healthcare Provider.
Q: What should I do if I experience complications with my IUD?
A: If you experience pain, unusual bleeding, or signs of infection, consult your healthcare provider immediately. Timely evaluation is essential to ensuring your health. More on this can be found in Addressing IUD Removal: What to Expect.
Q: How does an IUD compare to other contraceptive methods regarding fertility return?
A: IUDs generally allow for a swift return to fertility post-removal, comparable to other reversible methods like the pill or patch. Each method varies in how quickly fertility returns, so consider discussing all options with your healthcare provider, as mentioned in Comparing IUDs with Other Birth Control Methods.
Q: What are potential side effects of IUDs that could affect fertility?
A: While rare, complications like pelvic inflammatory disease or uterine perforation can potentially impact fertility. Understanding these risks and monitoring signs is crucial. For a deeper look into this topic, refer to Infertility and IUDs: Medical Opinions and Research.
Q: Can having an IUD removed affect my cycle or fertility?
A: The removal of an IUD often leads to normalization of your menstrual cycle, which can aid in conceiving. Individual experiences vary, and discussing your specific situation with a provider can provide clarity, especially in our Personal Stories: IUD Experiences and Fertility section.
Q: Is there a correlation between IUD use and the incidence of infertility?
A: No significant correlation exists between IUD use and infertility. Studies show that women who’ve used IUDs have similar fertility rates to those who’ve never used them. For further information, check The Science Behind IUDs and Fertility.
Wrapping Up
In summary, it’s essential to recognize that IUDs do not cause infertility and are a highly effective birth control option that can empower your reproductive choices without long-term concerns. If you’re considering your options, explore our articles on birth control alternatives and the safety and effectiveness of long-acting reversible contraception.
Take action today by reaching out for a consultation or signing up for our newsletter to stay informed on reproductive health topics relevant to your journey. Your path to understanding fertility is crucial, and we invite you to share your thoughts or questions in the comments below. Let’s navigate this together, ensuring you have the confidence and support you deserve as you make decisions about your body and future. Don’t miss out-explore our resources to gain insights into your health and well-being!





